Condition Basics
What is psoriasis?
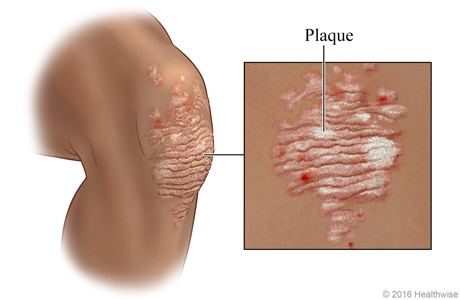
Psoriasis is a chronic skin condition that causes skin cells to grow too quickly. The result is thick white or red patches of skin. The patches (called plaques) can range in size from small to large. They usually occur on the knees, elbows, scalp, hands, feet, or lower back.
What causes it?
Experts believe that the immune system overreacts, causing inflammation and flaking of skin. In some cases, psoriasis runs in families. People with psoriasis often notice times when their skin gets worse. Things that can cause these flare-ups include a cold and dry climate, infections, stress, dry skin, and certain medicines.
What are the symptoms?
There are several types of psoriasis. Symptoms for each may vary. But major symptoms are itchy and tender skin and raised, bright red patches of skin (called plaques), topped with loose, silvery scales. In some people, psoriasis causes joints to become swollen, tender, and painful. Symptoms may disappear, even without treatment, and then return.
How is it diagnosed?
Your doctor can often recognize psoriasis by looking at your skin, scalp, and nails. Special tests usually aren't needed.
How is psoriasis treated?
Most cases of psoriasis are mild. Treatment starts with skin care. This includes keeping your skin moist with creams and lotions. These are often used with other treatments including shampoos, ultraviolet light, and medicines your doctor prescribes. You may need to try different combinations of treatments to find what works for you.
Cause
The exact cause of psoriasis isn't known. But experts believe that the immune system overreacts, causing inflammation and flaking of skin.
Many scientists believe that psoriasis can be inherited (runs in families). Having certain gene changes can make it more likely for a person to get psoriasis. But it isn't clear that your genes alone determine whether you get psoriasis.
People with psoriasis often notice times when their skin gets worse. Things that can cause these flare-ups include a cold and dry climate, infections, stress, dry skin, and taking certain medicines.
Psoriasis isn't contagious. It can't be spread by touch from person to person.
Symptoms
There are several types of psoriasis. Symptoms for each type may vary, but the major symptoms are:
- Raised, bright red patches of skin (called plaques). They're often covered with loose, silvery scales. They're usually on the knees, elbows, or low back.
- Tiny areas of bleeding when skin scales are picked or scraped off (Auspitz's sign).
- Mild scaling to thick, crusted plaques on the scalp.
- Itching, especially during sudden flare-ups or when the plaques are in body folds, such as under the breasts or buttocks.
- Discoloured or pitted nails.
Other symptoms may include:
- Similar plaques in the same area on both sides of the body.
- Flare-ups of many raindrop-shaped patches (guttate psoriasis).
- Joint swelling, tenderness, and pain (psoriatic arthritis).
- Psoriasis plaques that appear after an injury, such as a cut, a burn, or too much sun.
Symptoms may disappear (go into remission), even without treatment, and then return (flare up).
Learn more
What Happens
Psoriasis is usually a long-term problem. Symptoms tend to come and go in a cycle. There are flares, when symptoms get worse, and then remission, when symptoms improve and go away for awhile. In other cases, psoriasis may persist for long periods of time without getting better or worse.
A few flare-ups of psoriasis may go away without treatment. But it's usually best to treat psoriasis so that it doesn't get worse. If it becomes severe and widespread, it may be much harder to treat.
When to Call a Doctor
Call your doctor if you have:
- Symptoms of psoriasis. Early treatment may help keep the condition from getting worse.
- Signs of an infection, including:
- Increased pain, swelling, warmth, or redness.
- Red streaks leading from the area.
- Pus draining from the area.
- A fever.
If you are being treated for psoriasis, call your doctor if you:
- Have severe and widespread psoriasis and your skin is more irritated or inflamed than usual, especially if you have another illness.
- Are taking medicine for psoriasis and have serious side effects, such as vomiting, bloody diarrhea, chills, or a fever.
Examinations and Tests
Your doctor can often recognize psoriasis by looking at your skin, scalp, and nails.
Tests usually aren't needed. But one or more of the following tests may be done.
- Biopsy. If it's hard to diagnose the condition by looking at your skin, your doctor may remove a small skin sample and send it to a lab for analysis.
- X-rays. If you have joint pain, X-rays may be taken to look for psoriatic arthritis.
- Blood test. It can help rule out other forms of arthritis.
Treatment Overview
Most cases of psoriasis are mild and can be treated with:
- Creams, ointments, and lotions to moisturize the skin.
- Shampoos, oils, and sprays to treat psoriasis of the scalp.
- Some exposure to sunlight.
Depending on what type of psoriasis you have, treatment may also include:
- Skin products that your doctor prescribes.
- Pills that your doctor prescribes.
- Shots to help your immune system.
- Phototherapy. This involves exposing your skin to special ultraviolet light.
In some cases, psoriasis can be hard to treat. You may need to try different combinations of treatments to find what works for you. Treatment for psoriasis may go on for a lifetime.
Learn more
Self-Care
Most of the time psoriasis can be treated at home. These tips may improve your symptoms or help reduce the number of psoriasis flare-ups:
- Take care of your skin, scalp, and nails. For mild symptoms of psoriasis, various over-the-counter products, such as aloe vera, may be soothing and keep your skin moist.
- Try some of the many psoriasis creams, ointments, and shampoos that you can buy without a prescription.
- Follow your schedule for sunlight or ultraviolet light treatments.
- Try to eat a balanced diet and stay at a healthy weight.
- Be aware of possible medicine reactions. Certain medicines can trigger psoriasis or make symptoms worse.
- Avoid alcohol if it causes your symptoms to flare up.
What to avoid
You can do things at home to manage your psoriasis. By learning what triggers to avoid, you can improve your symptoms or help reduce the number of psoriasis flare-ups.
Try to avoid these triggers:
- Cold, dry climates. Cold weather may make symptoms worse. Hot, humid weather and sunlight may improve symptoms. (But hot, humid weather may make certain types of psoriasis worse.)
- Scratching and picking at your skin. Also avoid skin injuries (cuts or scrapes). An injury to the skin can cause psoriasis patches to form anywhere on the body, including the site of the injury. This includes injuries to your nails or nearby skin while trimming your nails.
- Infection. Infections such as strep throat can cause one type of psoriasis (called guttate psoriasis) to appear suddenly, especially in children.
- Stress and anxiety. Stress may cause psoriasis to appear suddenly (flare). Or it can make symptoms worse, although this has not been proved in studies.
- Smoking. Smoking can make your symptoms worse. If you smoke, consider quitting.
Explore more
Medicines
Many types of medicines can help control psoriasis. They include:
- Medicines you put on your skin (topical).
You may be able to control mild psoriasis with an over-the-counter medicine. These include corticosteroid creams.
For moderate to severe psoriasis, you may need to use a topical medicine prescribed by your doctor. For example, you may need a stronger corticosteroid or a medicine related to vitamin D.
Other topical medicines include anthralin and tars.
- Pills or shots.
Medicines you take by mouth may be used to treat moderate to severe psoriasis. Examples are retinoids and methotrexate.
Sometimes this type of medicine is given as shots instead of pills.
- Biologics.
These medicines block the harmful response of the body's immune system that causes the symptoms of psoriasis. These may be used to treat severe psoriasis. Or they may be used to treat psoriasis that hasn't improved after other treatments. Examples are infliximab (Remicade) and ustekinumab (Stelara).
Credits
Current as of: December 4, 2024
