Laparoscopic Adjustable Gastric Band Removal Surgery: What to Expect at Home
Your Recovery
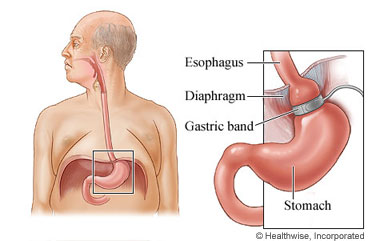
Lap band surgery (laparoscopic gastric banding) is surgery to help people lose weight. A gastric band creates a small pouch in the stomach. The pouch limits how much food you can eat. Surgery to remove a band might be done because the band didn't work as well as expected. In some cases, a band is removed because it slipped or eroded. When the band is removed, the doctor also removes the tube and port.
The cuts (incisions) the doctor made in your belly will probably be sore for a few days after the surgery. The stitches will dissolve on their own.
After this surgery, you may start to notice more feelings of hunger. And you may start to gain weight. You may be worried about weight gain. Your doctor can help you think about how you are feeling. You can discuss possible steps you can take to have a healthy weight.
Most people can return to their regular routines in 1 to 4 weeks after this surgery. Your doctor may give you specific instructions on when you can do your normal activities again, such as driving and going back to work.
This care sheet gives you a general idea about how long it will take for you to recover. But each person recovers at a different pace. Follow the steps below to get better as quickly as possible.
How can you care for yourself at home?
 Activity
Activity
- Rest when you feel tired.
- Be active. Walking is a good choice.
- Allow your body to heal. Don't move quickly or lift anything heavy until you are feeling better.
- Hold a pillow over your incisions when you cough or take deep breaths. This will support your belly and may help to decrease your pain.
- Do breathing exercises at home as instructed by your doctor. This will help prevent pneumonia.
- You will probably need to take 2 to 4 weeks off from work. It depends on the type of work you do and how you feel.
- You may shower, if your doctor okays it. Pat the incision dry. Do not take a bath for the first 2 weeks, or until your doctor tells you it is okay.
 Diet
Diet
- Your doctor will give you specific instructions about what to eat after the surgery. For the first few days, you will need to follow a liquid or soft diet. Bit by bit, you will be able to add solid foods back into your diet.
- Your doctor may recommend that you work with a dietitian to plan healthy meals.
- If your bowel movements are not regular right after surgery, try to avoid constipation and straining. Drink plenty of water. Your doctor may suggest fibre, a stool softener, or a mild laxative.
 Medicines
Medicines
- Be safe with medicines. Read and follow all instructions on the label.
- If the doctor gave you a prescription medicine for pain, take it as prescribed.
- If you are not taking a prescription pain medicine, ask your doctor if you can take an over-the-counter medicine.
- Your doctor will tell you if and when you can restart your medicines. You will also be given instructions about taking any new medicines.
- If you stopped taking aspirin or some other blood thinner, your doctor will tell you when to start taking it again.
 Incision care
Incision care
- If you have strips of tape on the incisions, leave the tape on for a week or until it falls off.
- Wash the area daily with warm water, and pat it dry. Don't use hydrogen peroxide or alcohol. They can slow healing.
- You may cover the area with a gauze bandage if it oozes fluids or rubs against clothing. Change the bandage every day.
- Keep the area clean and dry.
When should you call for help?
Call 911 anytime you think you may need emergency care. For example, call if:
- You passed out (lost consciousness).
- You are short of breath.
Call your doctor or nurse advice line now or seek immediate medical care if:
- You have pain that does not get better after you take pain medicine.
- You can't pass stools or gas.
- You are sick to your stomach or can't keep down fluids.
- You have loose stitches, or your incision comes open.
- You have signs of a blood clot in your leg (called a deep vein thrombosis), such as:
- Pain in your calf, back of the knee, thigh, or groin.
- Redness or swelling in your leg.
- You have signs of infection, such as:
- Increased pain, swelling, warmth, or redness.
- Red streaks leading from the incision.
- Pus draining from the incision.
- A fever.
Watch closely for changes in your health, and be sure to contact your doctor or nurse advice line if:
- You have new or worse symptoms of reflux.
- You have trouble or pain swallowing.
- You do not get better as expected.
Follow-up care is a key part of your treatment and safety. Be sure to make and go to all appointments, and call your doctor or nurse advice line (811 in most provinces and territories) if you are having problems. It's also a good idea to know your test results and keep a list of the medicines you take.
Where can you learn more?
Go to https://www.healthwise.net/patientEd
Enter L220 in the search box to learn more about "Laparoscopic Adjustable Gastric Band Removal Surgery: What to Expect at Home".
Current as of: March 1, 2025
