In 2013, 1 out of every 9 people in Alberta had osteoarthritis (OA). In the next 30 years, there could be over 10 million people in Canada with OA. This is mainly because:
- The population is getting older.
- People aren’t as fit as they used to be.
Learning more about your condition and taking an active part in your treatment are important. This information will help you understand your OA better and learn what you can do to manage it.
What is osteoarthritis?
Arthritis is a disease of the
joints (the areas where 2 bones meet). It often causes pain, swelling, and stiffness in your joints. It’s called a chronic disease because it doesn’t go away and a progressive disease because it can get worse. Osteoarthritis (OA) is the most common type of arthritis.
OA affects each person differently. Some have a lot of symptoms and joint changes, others don’t. OA can affect any joint, but it most commonly affects joints in your:
- hips
- knees
- hands and fingers
- spine
- feet and toes
- shoulders
Another type of arthritis is inflammatory arthritis, such as
rheumatoid arthritis. It’s possible to have more than one type.
What happens to the joint with OA?
OA happens when cartilage (tough elastic material that covers and protects the ends of bones) breaks down faster than your body rebuilds it. As cartilage breaks down, your bones rub together and damage your joint .
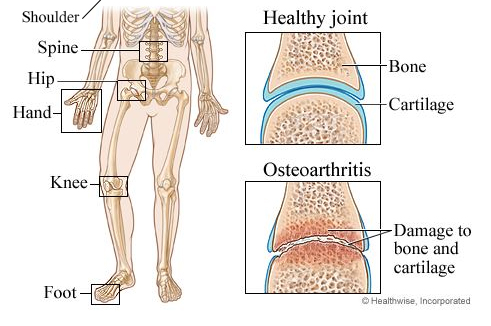
How osteoarthritis can damage joints.
Credit: Healthwise, Incorporated
This damage can cause pain, because bones contain nerves. Sometimes little bony growths, or spurs, develop on the ends of the bones.
OA causes swelling of your the joint capsule (tissue that encloses your joint) and ligaments (tough bands of flexible tissue that help hold your joint together). This swelling causes them to stretch. If this happens, the ligaments don’t go back to their original length. This can cause the joint to become unstable. You may hear your joints click, crunch, or crack.
Swelling and extra fluid in your joint can make it feel stiff and painful. Over time, the cartilage begins to fray and may even wear away entirely, causing your bones to rub against each other.
What are the symptoms of OA?
You can have OA in one joint or more than one. You may have some of the following symptoms:
- Your joints feel stiff when you get up in the morning.
- You have trouble moving or using your joints because of pain, stiffness, or swelling.
- Your joints ache during or after exercise.
- You hear more cracking, creaking, or crunching when you move your joints.
How is OA diagnosed?
To know if you have OA, your healthcare provider will examine you, ask you about your symptoms, and talk to you about your risk factors for OA. Most people
don’t need an MRI (magnetic resonance imaging) or x-rays to diagnose OA.
What are the risk factors?
Here are some of the risk factors for OA:
- Joint injuries: Having an injury can put you at higher risk for developing OA in that joint or nearby joints.
- Repetitive movements: Repeating the same movements over and over can put stress on your joints and lead to OA. For example, jobs where you need to do a lot of squatting, gripping, or kneeling may raise your risk of OA.
- Weight: Stay at a healthy body weight so there’s no extra force on your joints. For every extra pound of body weight, there’s 4 to 6 times more force through your knee joints.
- Age: OA is more common in people older than 40.
- Sex: OA is more common in females.
- Family history: You may have a higher risk of OA if your parent or sibling has it.
