Condition Basics
What is a meniscus tear?
A meniscus tear is a common knee injury. The meniscus is a rubbery, C-shaped disc that cushions your knee. Each knee has two menisci (plural of meniscus)—one at the outer edge of the knee and one at the inner edge. They keep your knee steady by balancing your weight across the knee. A torn meniscus can prevent your knee from working right.
What causes it?
A meniscus tear is usually caused by twisting or turning quickly, often with your foot planted while your knee is bent. Meniscus tears can occur when you lift something heavy or play sports. As you get older, your meniscus gets worn. This can make it tear more easily.
What are the symptoms?
Symptoms of a meniscus tear depend on the size and location of the tear. They also depend on your age and the health of your knee. A tear can cause pain, swelling, and stiffness. The knee may catch, pop, or lock. It may be hard to walk.
How is it diagnosed?
Your doctor will ask questions about your knee and what you were doing when it started to hurt. Your doctor will look at both knees and check for tenderness and range of motion and see how stable your knee is. You may also have other tests, such as X-rays or an MRI.
How is a meniscus tear treated?
Treatment may include resting your knee, using ice on it, wrapping it with an elastic bandage, and propping it up on pillows. It may also include physiotherapy and surgery. Your treatment depends on the type of tear, where it is, and how serious it is. It also depends on your age and how active you are.
Symptoms
Symptoms of a meniscus tear depend on the size and location of the tear. They also depend on your age and the health of your knee.
Symptoms may include things like knee pain, swelling, or stiffness. It may be hard to walk. Your knee may feel unstable, or it may be hard to straighten all the way. Or you may feel like your knee "catches" when you move.
Some people have severe pain and swelling right away when the tear happens. Or they might have less pain and swelling at first but then notice that it gets worse over a few days.
Older people sometimes don't notice when the tear happens. But then they notice symptoms later.
What Happens
What happens depends on the size of the tear, its location, and your symptoms. It also depends on whether your knee was healthy when the tear happened, or if your knee already had age-related changes.
Tears caused by an injury in younger people may heal over time with rest and physiotherapy. Surgery is often used for large tears. That's because they can lead to long-term problems if they aren't repaired.
When the tear is in a knee that has age-related changes, symptoms may be helped by rest, physiotherapy, and time. In some cases, a doctor may suggest surgery.
How the location and type of tear affect healing
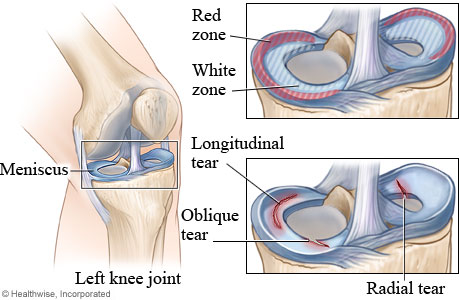
Where a meniscus tear occurs is one of the most important things that affects healing. Tears at the outer edge (red zone) tend to heal well because there is a good blood supply. The inner area (white zone) lacks a good blood supply and therefore does not heal well.
The type of tear often determines whether a tear can be repaired. Longitudinal tears are often repairable. Radial tears may be repairable depending on where they are located. Oblique (flap) tears and another type called horizontal tears are generally not repairable.
When to Call
Check your symptoms
Examinations and Tests
Your doctor will ask about past injuries and what you were doing when your knee started to hurt. A physical exam will help your doctor find out if a torn meniscus is the cause of your pain. Your doctor will look at both knees and check for tenderness and range of motion and see how stable your knee is.
You may have tests such as X-rays to check the bones of the knee or an MRI, which can give a clear picture of where a tear is and how it might be treated. The doctor may order the MRI if the diagnosis is not clear. You may need to meet with an orthopedic surgeon.
Learn more
Watch
Treatment Overview
Your choices for treating a torn meniscus are:
- Treatment without surgery. This includes resting, using ice, wrapping the knee in an elastic bandage, propping it up on pillows, and doing physiotherapy. This treatment choice may include wearing a temporary knee brace.
- Surgery to sew the tear together.
- Surgery to remove the torn section of the meniscus.
- Surgery to remove the entire meniscus.
There are many things to think about when deciding how to treat a torn meniscus. These things include where the tear is and how serious it is, your pain level, your age and activity level, your doctor's preference, and when the injury happened. The decision about whether to have surgery depends on the kinds of symptoms you have and how bad they are, not just on how big the tear is. You may have a large tear but still decide not to have it repaired.
Meniscus repair is more successful if:
- You are younger. Experts think people younger than about age 40 do best.footnote 1
- Your knee has good stability from the ligaments.
- The tear is in the outer edge of the meniscus.
- The repair is done soon after the injury.
Learn more
Self-Care
If you have a new meniscus tear or a flare-up of severe pain from a tear, you can take these steps to reduce pain and swelling:
- Rest and reduce your activity. Avoid motions or positions that cause discomfort. Follow your doctor's directions for using crutches or a knee brace, if suggested.
- Put ice or a cold pack on your knee for 10 to 20 minutes at a time. Try to do this every 1 to 2 hours for the next 3 days (when you are awake) or until the swelling goes down. Put a thin cloth between the ice and your skin.
- Wrap the knee with an elastic bandage, such as an Ace wrap, to help decrease swelling.
- Prop up the sore leg on a pillow when you ice your knee or anytime you sit or lie down during the next 3 days. Try to keep your leg above the level of your heart. This will help reduce swelling.
- Ask your doctor if you can take NSAIDs, such as ibuprofen or naproxen, to relieve pain and reduce swelling. Be safe with medicines. Read and follow all instructions on the label.
- Follow your doctor's instructions for resting and caring for your knee.
If you have ongoing pain from a meniscus tear, you can work with your doctor to plan a rehabilitation (rehab) program that helps you regain as much strength and flexibility in your knee as possible. Your rehab program probably will include physiotherapy and home exercises.
- A program of physiotherapy and home exercises can help your knee heal and help you return to your activities.
- Building strength and flexibility in your knee and legs may help prevent future degeneration in your knee.
Learn more
Watch
Surgery
When you have a meniscus tear, your doctor may recommend surgery if home care and rehab haven't helped. Your choices are:
- Surgery to sew the tear together.
- Surgery to remove the torn section of the meniscus.
- Surgery to remove the entire meniscus.
Whenever possible, meniscus surgery is done using arthroscopy, rather than through a large cut in the knee.
Your doctor will likely suggest the treatment that they think will work best for you. This is based on where the tear is, the pattern of the tear, and how big it is.
Your pain level, your age, your health, and your activity level may also affect your treatment options.
Extent and success of meniscus repair
It's best to keep as much of the meniscus as possible. If the meniscus can be repaired successfully, repairing it reduces the chance of knee joint degeneration compared with removing all or part of the meniscus.
Meniscus repair is more successful if:
- You are younger. Experts think people younger than about age 40 do best.footnote 1
- Your knee has good stability from the ligaments.
- The tear is in the outer edge of the meniscus.
- The repair is done soon after the injury.
Meniscal repair may prevent degenerative changes in the knee joint. Many doctors believe that a successful meniscus repair lowers the risk of early-onset arthritis, because it reduces the stress put on the knee joint.
Other surgery option
Meniscal transplant is another treatment for painful meniscus problems. It's often only done if you've already had part or all of your meniscus removed and don't have arthritis in your knee.
Learn more
Watch
References
Citations
- Wynkoop A, et al. (2021). Sports medicine: Lower extremity. In PJ McMahon, HB Skinner, eds., Current Diagnosis and Treatment in Orthopedics, 6th ed. New York: McGraw Hill. Accessed June 24, 2021.
Credits
Current as of: July 31, 2024
