Follow your medication instructions. Your surgeon, or the Pre-Admission Clinic nurses or doctors will tell you what medication you can take on the day of surgery.
Most patients go home the same day of surgery. Your support person may need to take care of your personal belongings and give them to you after surgery. How long you stay in hospital will depend on the type of surgery and your recovery.
If you’ve had surgery before, you may notice a few things that are different about your surgery.
What do I bring?
What to bring on the day of your surgery (your Operating Room day):
- Alberta Health card and your Blue Cross or other insurance card
- Photo identification (please make sure the information is correct)
-
Your Journey Through Breast Cancer Surgery book (PDF), along with any handouts you were given about your condition or surgery
- All your medication (in original containers) including inhalers, aspirin, vitamins, herbal and over-the-counter medications (a list from your pharmacy would be helpful)
- CPAP / BiPAP machine (if you use it, as it may be sent to the recovery room during your surgery)
- Proof of medical coverage (out-of-province residents only)
Personal care items to bring:
- Items your surgeon has requested
- Walking aids such as a walker or cane (if you use one)
- Comfortable clothing. You may not want to wear a bra right after breast-conserving surgery. If you need support, you may find a front-opening bra or camisole more comfortable. Bring a loose-fitting button or zip-up top to wear home – reaching overhead may be difficult. Do not wear tight-fitting or underwire bras.
- Ear plugs
- Hearing aids, eyeglasses, dentures and denture case
- Book, magazine or something else to keep you busy
Do not bring:
- Anything of value (jewellery, credit cards)
- More than $20 cash
- A tablet or computer
- Electrical appliances such as hair dryers or curling irons
Rules about using cell phones in the hospital are different on each unit. Ask your nurse before using your phone.
Bring these items in 1 small bag that has your name on it. Please leave these items with your support person who can give these to you after surgery.
At the hospital
When you arrive at the hospital, a nurse will:
- Go through a list of questions with you.
- Ask you to change into a hospital gown.
You may be given some medicine with a sip of water before surgery to help lower your pain and nausea.
Holding area
You’ll be brought to an area outside of the operating room (holding area) where you’ll meet your surgical team: your anesthesiologist (the doctor who will give you medicine to keep you asleep during your surgery), surgeon, and nurses.
While you’re in the area outside of the operating room, a nurse will ask you questions from the Safe Surgery Checklist such as your name, surgery, birthdate, allergies, and what surgery you’re having. You may be asked this more than once, which is normal. Your healthcare team does this to keep you safe.
An intravenous (IV) will be started before or when you’re in the operating room. This is a plastic tube that is placed in your vein to give you medicine and fluid during and after surgery.
Waiting area
Visitors may be restricted depending on the situation. If your support person is not able to wait for you in the waiting area, staff will call them to let them know when your surgery is finished and they can return.
Operating room
An operating room nurse will double-check your surgical information and take you into the operating room. The Safe Surgery Checklist will be repeated.
The anesthesiologist will give you medicine (general anesthetic) to make you comfortable and keep you asleep during your surgery.
Your surgery will take:
- about 1 to 2 hours (without reconstruction)
- 2 to 7 hours (if you’re having breast reconstruction at the same time)
What else do I need to know?
- If a yellow or blue band is put on your wrist, do not take it off. You will need to have another blood sample otherwise, which may delay your surgery.
- Usually only 1 person can stay with you until you go to surgery. Visitors policies can change in different situations.
Procedures before and during surgery
-
Wire/seed localization. To help guide the surgeon, you may have a seed or wire localization.
-
Sentinel lymph node mapping. Will be done either the day before your surgery or the morning of your surgery.
-
Intravenous (IV). An IV is started in your hand or arm by the nurse before you go to the operating room, or by the anesthesiologist in the operating room. It’s used to give the anaesthetic (sleeping medicine) and other medication you may need such as antibiotics. The IV is usually taken out once you are able to drink well after surgery.
-
Medication. You may be given medication before you go to the operating room or in the operating room before the surgery begins. You may need to continue taking this medication after surgery:
- IV antibiotics to protect against infection
- Medications to prevent nausea and pain
-
Air-filled stockings (sequential compression device). You may wear compression stockings on your legs during and after your operation to promote blood flow in your legs and help to prevent blood clots. A machine inflates and deflates the stockings. They are taken off once you are walking around.
-
Blood transfusion. Not many people need a blood transfusion. If you need to have blood, your surgeon will talk with you.
After surgery (in hospital)
After surgery, you’ll be moved to the recovery room, where you will stay for 1 to 3 hours. Visitors are not allowed in the recovery room. You’ll stay there until your healthcare team decides it’s safe for you to go to the Day Surgery Unit or a surgical unit.
What to expect
You will probably feel sleepy and your throat may feel sore from the tube that was placed in it while you were asleep. This is normal. You will also have:
- an IV to give you fluid and medicine. You may be given medicines to help with your pain and nausea. As soon as you can, your healthcare team will ask you to start drinking fluids.
- a dressing (bandage) on your chest. It’s important not to touch your dressing to allow for proper healing.
- you may have 1 or more drains near the area where the incision was made. Drains take extra fluid away from below your incision.
Your nurse will regularly check your:
- Heart rate, breathing, blood pressure, and blood oxygen level
- Dressing (bandage)
- Drains
- Pain and nausea levels
Eating and drinking
You can eat solid food when you are able to. Your nutrition is an important part of healing. Start with a bit of soft food and when you move to solid food,
eat a nutritious, well-balanced diet.
Managing pain and nausea
Managing pain and nausea is important. It helps you recover sooner because you will:
- Breathe and move better
- Find it easier to eat and drink
- Sleep better
Pain after surgery is normal. You may have pain, numbness, or tingling in your shoulder, arm, armpit, or incision area. The type of pain you have and how long it lasts is different for everyone. A feeling of stabbing pain may happen and is normal.
Your healthcare team will give you pain or nausea medicine by IV, injection, or pill as needed while you’re in the hospital. Your nurse will ask you to rate your pain and nausea from 0 (no pain) to 10 (the worst pain you can imagine). Tell your nurse when you’re having pain or nausea. The amount of pain medicine will be adjusted as needed.
Dressings and incisions
The size of your incision (surgical cut) and where it is will depend on where your cancer was and the type of breast surgery you had. You may have a breast incision and an underarm incision.
At first, you’ll have an outer gauze dressing (bandage) covering the incisions. Gauze dressings usually stay on for 24 to 48 hours. Your surgeon will tell you when you can take your dressing off.
Your incisions are held together with staples or stitches (sutures) and covered with Steri-strips (paper or surgical tapes). The surgeon will tell you when your Steri-strips can be removed. Dissolving stitches are used most often and don’t need to be removed.
If you have a clear, sticky dressing, it will stay on for 2 to 7 days. Your surgeon will tell you when you can take it off.
Drains
A drain is a small plastic tube inserted through the skin near the incision. It’s stitched in place so it doesn’t fall out. A small plastic suction container is attached to it. After breast surgery, it‘s normal for your body to make extra fluid in the area around your incision. The drains remove this extra fluid and blood. Removing the fluid helps with healing and lowers the risk of infection.
Depending on the surgery you may not have a drain at all, or may have 1 or 2 drains in place.
The drains most commonly used are the Jackson-Pratt and the Blake. Your healthcare team can tell you what kind of drain you have. Write this information down on
My Plan. They will teach you how to care for your drain(s) before you leave the hospital.
Find more information on
how to care for your drain at home.
Getting moving and doing leg exercises
Be active as soon as possible. Moving and doing leg exercises will help you build strength, increase blood flow, prevent clots from forming and keep your lungs clear. Your nurse will help you get up to walk soon after surgery.
- Move and stretch your legs
- Wiggle your toes
- Change position in bed
- Get up to sit in a chair
- Do basic leg exercises
- Walk
- Increase your activity level gradually after surgery (no strenuous exercise).
Symptoms of a blood clot may include any of the following:
- Swelling
- Redness
- Warmth to skin
- Pain to 1 or both legs
- Shortness of breath
Let the medical team know right away if you have any of these symptoms.
Do not massage your leg if you are having these symptoms. You could cause the clot to break off.
Leg exercises
Do these exercises 5 times each hour you are awake. These can be done lying in bed or sitting in a chair.
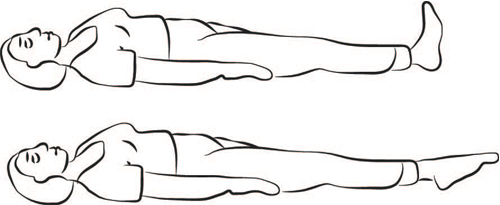
Flex your feet up and down for 1 minute. Relax. Repeat.
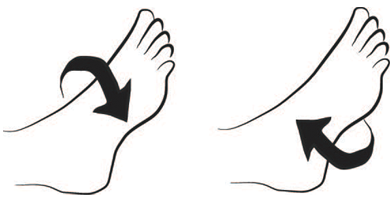
Make circles with your feet. Repeat in the other direction.
Deep breathing and coughing exercises
It’s important to do your deep breathing and coughing exercises if you have had an anesthetic and to prevent lung infections.
Follow these steps 1 time every hour you are awake:
- Breathe in deeply through your nose.
- Hold your breath for 5 to 10 seconds, and then breathe out slowly through your mouth. You will be able to breathe more deeply with each breath.
- Repeat again.
- Repeat again. This time, hold your breath for 5 to 10 seconds. Cough 2 or 3 times in a row as you get rid of this breath.
- Make sure you take normal breaths when you’re not doing these exercises.
- Ask your healthcare team if you should do these exercises more often or less often than 1 time every hour.
Using your arm
After surgery, try to use your arm on the side of your surgery as you normally would (for eating, drinking, brushing your teeth and hair, answering the phone). It’s important to move it regularly.
Keep good posture. When using your arm, it is important to make sure you have good posture. Keep your shoulders back and down. If you are lifting your arm overhead, try to keep your shoulders back and down.
Learn more about
arm and shoulder exercises.
Going home (discharge) checklist
Before you’re sent home, your healthcare team will:
- Review your discharge instructions with you.
- Give you the date for your follow-up appointment
or tell you when to call your surgeon’s office to make your follow-up appointment. Write this on
My Plan.
- Give you prescriptions for medicines to take at home and instructions on when you can take your regular medicines.
- Ask you if you have arranged for someone to drive you home and stay with you for 24 hours after your surgery.
- Tell you when you can have a shower. Write this down on
My Plan.
- Make a referral to home care if needed. Most people don’t need home care.
Talk to your healthcare team if you feel something on this list hasn’t been done.
